Новая область применения слюны в прогностических целях на примере рака легких
1Научно-исследовательская лаборатория биохимии, Омский государственный педагогический университет, 644043, Омск, ул. Наб. Тухачевского, 14, *e-mail: belskaya@omgpu.ru
2Кафедра онкологии, Омский государственный медицинский университет, 644099, Омск, ул. Ленина, 12
Ключевые слова:слюна; биохимический состав; рак легкого; общая выживаемость; прогноз; аденокарцинома; плоскоклеточная карцинома; нейроэндокринный рак
DOI:10.18097/BMCRM00133
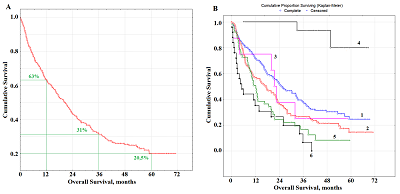
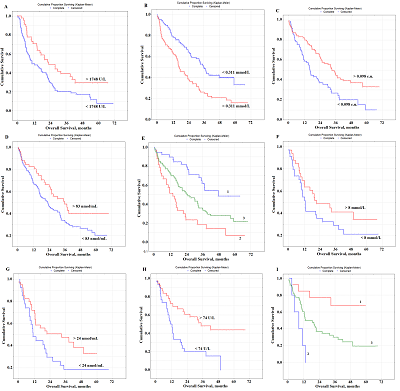
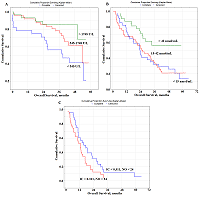
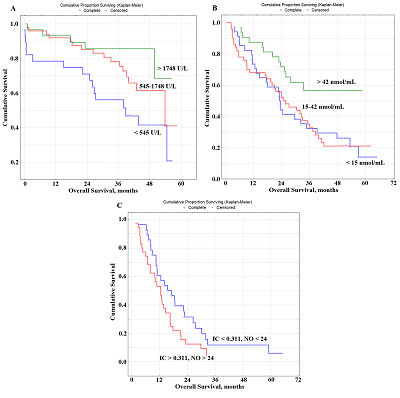
Целью данной работы было определение потенциальной прогностической роли биохимических показателей слюны при раке легкого. В исследование включены 425 больных раком легких различных гистологических типов. Перед лечением были собраны образцы слюны и определены 34 биохимических параметра. Прогностические факторы были проанализированы с помощью многомерного анализа с использованием модели пропорциональных рисков Кокса. Полученные результаты свидетельствуют о том, что для плоскоклеточного рака независимым прогностически неблагоприятным фактором является активность лактатдегидрогеназы (ЛДГ) менее 1748 Е/л (отношение рисков (ОР) = 2,89; 95% доверительный интервал (ДИ) 1,28 – 6,46; р = 0,00330). Для аденокарциномы можно выделить сочетание нескольких факторов: содержание имидазольных соединений более 0,311 ммоль/л, серомукоидов менее 0,098 у.е. и мочевой кислоты менее 83 нмоль/мл (ОР = 7,91; 95% ДИ 2,52 – 24,11; р = 0,00004). Для нейроэндокринного рака легкого неблагоприятный прогноз связан с содержанием мочевины менее 8 ммоль /л, NO менее 24 нмоль/мл и активностью щелочной фосфатазы менее 74 Е/л (ОР = 12,50; 95% ДИ 1,09–138,7; р = 0,01184). Для радикального лечения неблагоприятный прогноз связан с активностью ЛДГ менее 545 Е/л (ОР = 7,20; 95% ДИ 2,13 – 23,70; p = 0,00968), для комбинированного лечения с уровнем NO менее 15 нмоль/мл (ОР = 5,64; 95% ДИ 1,89 – 16,46; p = 0,02797). Наихудший прогноз для паллиативного лечения наблюдается при уровне NO менее 24 нмоль/мл и содержании имидазольных соединений более 0,311 ммоль/л (ОР = 2,73; 95% ДИ 1,07 – 12,92; р = 0,01827). Выявленные параметры могут быть использованы для прогнозирования рака легких и корректировки тактики лечения пациентов.
|
ЗАКРЫТЬ

|
Таблица 1.
Описание исследуемой группы
|
|
ЗАКРЫТЬ

|
Таблица 2.
Анализ переменных, влияющих на общую выживаемость больных раком легких
|
|
ЗАКРЫТЬ

|
Таблица 3.
Анализ биохимических параметров слюны, влияющих на общую выживаемость пациентов с раком легкого
|
БЛАГОДАРНОСТИ
Работа выполнена при финансовой поддержке Омского государственного медицинского университета и Омского государственногопедагогическогоуниверситета
ДОПОЛНИТЕЛЬНЫЕ МАТЕРИАЛЫ
К данной статье приложены дополнительные материалы, свободно доступные в электронной версии (http://dx.doi.org/10.18097/BMCRM00133) на сайте журнала.
ЛИТЕРАТУРА
- Bray, F., Ferlay, J., Soerjomataram, I., Siegel, R.L., Torre, L.A., Jemal, A. (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries, 68(6), 394–424. DOI
- Global Burden of Disease Cancer Collaboration. (2019) Global, Regional, and National Cancer Incidence, Mortality, Years of Life Lost, Years Lived with Disability and Disability-Adjusted Life-Years for 29 Cancer Groups, 1990 to 2017. A Systematic Analysis for the Global Burden of Disease Study. JAMA Oncology, DOI
- Okiror, L., Harling, L., Toufektzian L., King J., Routledge T., Harrison-Phipps K., Pilling, J., Veres, L., Lal, R., Bille, A. (2018) Prognostic factors including lymphovascular invasion on survival for resected non-small cell lung cancer. The Journal of Thoracic and Cardiovascular Surgery, 156(2), 785–93. DOI
- Molinier, O., Goupil, F., Debieuvre, D., Auliac, J-B., Jeandeau, S., Lacroix, S., Martin, F. Grivaux, M. (2019) Five-year survival and prognostic factors according to histology in 6,101 Non-Small-Cell Lung Cancer patients. Respir Med Res, 77, 46–54. DOI
- Grosu, H.B., Manzanera, A., Shivakumar, S., Sun, S., Gonzalez Graciela, N., Ost, E. (2020) Survival disparities following surgery among patients with different histological types of non-small cell lung cancer. Lung Cancer, 140, 55–8. DOI
- Soliman, S.E., Alhanafy, A.M., Habib, M.S.E., Hagag, M., Ibrahem, R.A.L. (2018) Serum circulating cell free DNA as potential diagnostic and prognostic biomarker in non-small cell lung cancer. Biochemistry and Biophysics Reports, 15, 45–51. DOI
- Sandfeld-Paulsen, B., Aggerholm-Pedersen, N., Bæk, R., Jakobsen, K.R., Meldgaard, P., Folkersen, B.H., Rasmussen, T.R., Varming, K., Jørgensen, M.M., Sorensen, B.S. (2016) Exosomal proteins as prognostic biomarkers in non-small cell lung cancer. Molecular Oncology, 10, 1595–602. DOI
- Pérez-Ramírez, C., Cańadas-Garre, M., Alnatsha, A., Molina, M.Á., Robles, A.I., Villar, E., Delgado, J.R., Faus-Dáder, M.J., Calleja-Hernández, M.Á. (2017) Interleukins as new prognostic genetic biomarkers in non-small cell lung cancer. Surgical Oncology, 26, 278–85. DOI
- Targowski, T., Jahnz-Rozyk, K, Owczarek, W, Raczka, A, Janda, P, Szkoda, T, Płusa, T. (2010) Telomerase activity and serum levels of p53 protein as prognostic factors of survival in patients with advanced non-small cell lung cancer. Respiratory Medicine, 104, 1356–61. DOI
- Chen, S., Yan, H., Du, J., Li, J., Shen, B., Ying, H., Zhang, Y., Chen, S. (2018) Prognostic significance of pre-resection albumin/fibrinogen ratio in patients with non-small cell lung cancer: A propensity score matching analysis. Clinica Chimica Acta, 482, 203–8. DOI
- Koh, Y.W., Lee, S.J., Park, S.Y. (2017) Prognostic significance of lactate dehydrogenase B according to histologic type of non-small-cell lung cancer and its association with serum lactate dehydrogenase. Pathology – Research and Practice, 213(9), 1134–8. DOI
- Hermes, A., Gatzemeier, U., Waschki, B., Reck, M. (2010) Lactate dehydrogenase as prognostic factor in limited and extensive disease stage small cell lung cancer - A retrospective single institution analysis. Respiratory Medicine, 104, 1937–42. DOI
- Li, S-J., Lv, W-Y., Du, H., Li, Y-J., Zhang, W-B., Che, G-W., Liu, L.X. (2019) Albumin-to-alkaline phosphatase ratio as a novel prognostic indicator for patients undergoing minimally invasive lung cancer surgery: Propensity score matching analysis using a prospective database. International Journal of Surgery, 69, 32–42. DOI
- Yang, Z., Li, S., Zhao, L., Lv, W., Ju, J., Zhang, W., Li, J., Che, G. (2020) Serum uric acid to lymphocyte ratio: a novel prognostic biomarker for surgically resected early-stage lung cancer. A propensity score matching analysis. Clinica Chimica Acta, 503, 35-44. DOI
- Tanriverdi, O., Cokmert, S., Oktay, E., Pilanci, K.N., Menekse, S., Kocar, M., Sen, C.A., Avci, N., Akman, T., Ordu, C., Goksel, G. Meydan, N. (2014) Prognostic significance of the baseline serum uric acid level in non-small cell lung cancer patients treated with first-line chemotherapy: a study of the Turkish Descriptive Oncological Researches Group. Med Oncol, 31(10), 217. DOI
- Pietrzak, S., Wojcik, J., Scott, R.J., Kashyap, A., Grodzki, T., Baszuk, P., Bielewicz, M., Marciniak, W., Wójcik, N., Dębniak, T., Masojć, B., Pieróg, J., Cybulski, C., Gronwald, J., Wojtyś, M., Kubisa, B., Sukiennicki, G., Deptuła, J., Waloszczyk, P., Jakubowska, A., Lubiński, J., Lener, M.R. (2019) Influence of the selenium level on overall survival in lung cancer. Journal of Trace Elements in Medicine and Biology, 56, 46–51. DOI
- Liu, Y., Gu, X., Lin, Q., Tian, T., Shao, L., Yuan, C., Zhang, B., Fan, K. (2015) Prognostic significance of osteopontin in patients with non-small cell lung cancer: results from a meta-analysis. Int J Clin Exp Med, 8(8), 12765–73.
- Ilie, M., Mazure, N.M., Hofman, V., Ammadi, R.E., Ortholan, C., Bonnetaud, C., Havet, K., Venissac, N., Mograbi, B., Mouroux, J., Pouysségur, J., Hofman, P. (2010) High levels of carbonic anhydrase IX in tumour tissue and plasma are biomarkers of poor prognostic in patients with non-small cell lung cancer. Br J Cancer, 102, 1627–35. DOI
- Dehing-Oberije, C., Aerts, H., Yu, S., De Ruysscher, D., Menheere, P., Hilvo, M.,van der Weide, H., Rao, B., Lambin, P. (2011) Development and validation of a prognostic model using blood biomarker information for prediction of survival of non-small-cell lung cancer patients treated with combined chemotherapy and radiation or radiotherapy alone (NCT00181519, NCT00573040, and NCT00572325). Int J Radiat Oncol Biol Phys, 81(2), 360-368. DOI
- Gomes, M., Coelho, A., Araujo, A., Azevedo, A., Teixeira, A.L., Catarino, R., Medeiros, R. (2015) IL-6 polymorphism in non-small cell lung cancer: a prognostic value? Tumour Biol, 36, 3679–84. DOI
- Sanmamed, M.F., Carranza-Rua, O., Alfaro, C., Onate, C., Martin-Algarra, S., Perez, G., Landazuri, S.F., Gonzalez, A., Gross, S., Rodriguez, I., Muñoz-Calleja, C., Rodríguez-Ruiz, M., Sangro, B., López-Picazo, J.M., Rizzo, M., Mazzolini, G., Pascual, J.I., Andueza, M.P., Perez-Gracia, J.L., Melero I. (2014) Serum interleukin-8 reflects tumor burden and treatment response across malign ancies of multiple tissue origins. Clin Cancer Res, 20, 5697–707. DOI
- De Vita, F., Orditura, M., Galizia, G., Romano, C., Roscigno, A., Lieto, E., Catalano, G. (2000) Serum Interleukin-10 Levels as a Prognostic Factor in Advanced Non-small Cell Lung Cancer Patients. CHEST, 117(2), 365–73. DOI
- Fiala, O., Pesek, M., Finek, J., Topolcan, O., Racek, J., Minarik, M., Benesova, L., Bortlicek, Z., Poprach, A. Buchler, T. (2015) High serum level of C-reactive protein is associated with worse outcome of patients with advanced-stage NSCLC treated with erlotinib. Tumour Biol, 36, 9215–22. DOI
- Machado, D., Marques, C., Dias, M., Campainha, S., Barroso, A. (2019) Inflammatory prognostic biomarkers in advanced non-small cell lung cancer. Pulmonology, 25(3), 181–3. DOI
- Zhang, Z.H., Han, Y.W., Liang, H., Wang, L.M. (2015) Prognostic value of serum CYFRA21-1 and CEA for non-small-cell lung cancer. Cancer Med, 4, 1633–8. DOI
- Hanagiri, T., Sugaya, M., Takenaka, M., Oka, S., Baba, T., Shigematsu, Y., Nagata, Y., Shimokawa, H., Uramoto, H., Takenoyama, M., Yasumoto, K., Tanaka, F. (2011) Preoperative CYFRA 21-1 and CEA as prognostic factors in patients with stage I non-small cell lung cancer. Lung Cancer, 74, 112–7. DOI
- Carvalho, S., Troost, E.G.C., Bons, J., Menheere, P., Lambin, P., Oberije, C. (2016) Prognostic value of blood-biomarkers related to hypoxia, inflammation, immune response and tumour load in non-small cell lung cancer – A survival model with external validation. Radiotherapy and Oncology, 119(3), 487–94. DOI
- Chiappin, S., Antonelli, G., Gatti, R., De Palo, E.F. (2007) Saliva specimen: a new laboratory tool for diagnostic and basic investigation. Clinica Chimica Acta, 383, 30-40. DOI
- Punyadeera, C., Slowey, P.D. (2019) Saliva as an emerging biofluid for clinical diagnosis and applications of MEMS/NEMS in salivary diagnostics. Nanobiomaterials in Clinical Dentistry, 22, 543-65. DOI
- Roblegg, E., Coughran, A., Sirjani, D. (2019) Saliva: An all-rounder of our body. European Journal of Pharmaceutics and Biopharmaceutics, 142, 133–41. DOI
- Bel’skaya, L.V. (2019) Possible applications of saliva for the diagnosis of cancer. Russian Сlinical Laboratory Diagnostics, 64(6), 333-6. DOI
- Zhang, L., Xiao, H., Zhou, H., Santiago, S., Lee, J.M., Garon, E.B., Yang, J., Brinkmann, O., Yan, X., Akin, D., Chia, D., Elashoff, D., Park, N., Wong, D.T.W. (2012) Development of transcriptomic biomarker signature in human saliva to detect lung cancer. Cellular and Molecular Life Sciences, 69(19), 3341–50. DOI
- Kisluk, J., Ciborowski, M., Niemira, M., Kretowski, A., Niklinski, J. (2014) Proteomics biomarkers for non-small cell lung cancer. Journal of Pharmaceutical and Biomedical Analysis, 101, 40-9. DOI
- Sun, Y., Liu, S., Qiao, Z., Shang, Z., Xia, Z., Niu, X., Qian L., Zhang Y., Fan L., Cao C.-X., Xiao H. (2017) Systematic comparison of exosomal proteomes from human saliva and serum for the detection of lung cancer. Anal Chim Acta, 982, 84-95. DOI
- Bel’skaya, L.V., Kosenok, V.K., Massard, G. (2016) Endogenous Intoxication and Saliva Lipid Peroxidation in Patients with Lung Cancer. Diagnostics, 6(4), 39. DOI
- Bel’skaya, L.V., Kosenok, V.K., Sarf, E.A. (2017) Chronophysiological features of the normal mineral composition of human saliva. Arch. Oral Biol, 82, 286–92. DOI
- Dos Santos, D.R., Souza, R.O., Dias, L.B., Ribas, T.B., Farias de Oliveira, L.C., Sumida, D.H., Dornelles, R.C.M., de Melo, A.C., Nakamune, S., Chaves-Neto, A.H. (2018) The effects of storage time and temperature on the stability of salivary phosphatases, transaminases and dehydrogenase. Arch. Oral Biol, 85, 160–5. DOI
- Bel’skaya, L.V., Sarf, E.A., Solonenko, A.P. (2019) Morphology of Dried Drop Patterns of Saliva from a Healthy Individual Depending on the Dynamics of Its Surface Tension. Surfaces, 2(2): 395-414. DOI
- Bel’skaya, L.V., Kosenok, V.K., Massard, G. (2019) Antioxidant protection system in the saliva of patients with non-small cell lung cancer. Biomedical Chemistry: Research and Methods, 2(1), e00061. DOI
- Bel’skaya, L.V., Kosenok, V.K. (2017) The activity of metabolic enzymes in the saliva of lung cancer patients. Natl J Physiol Pharm Pharmacol, 7(6), 646-53. DOI
- Savchenko, A.A., Lapeshin, P.V., Dykhno Y.A. (2004) Dependence of the activity of metabolic enzymes of blood lymphocytes in the cells of healthy and tumor lung tissue in patients with lung cancer. Russian Biotherapeutic Journal, 4(3), 70-75. DOI
- Wang, Z-X., Yang, L-P., Qiu, M-Z., Wang, Z-Q., Zhou, Y-X., Wang, F., Zhang, D-S., Wang, F-H., Li, Y-H., Xu, R-H. (2016) Prognostic value of preoperative serum lactate dehydrogenase levels for resectable gastric cancer and prognostic nomograms. Oncotarget, 26(7), 945-56. DOI
- Yao, F., Zhao, T., Zhong, C., Zhu, J., Zhao, H. (2013) LDHA is necessary for the tumorigenicity of esophageal squamous cell carcinoma. Tumor Biology, 34, 25-31. DOI
- Huijgen, H.J., Sanders, G., Koster, R.W., Vreeken, J., Bossuyt, P. (1997) The clinical value of lactate dehydrogenase in serum: a quantitative review. Eur Clin Chem Clin Biochem, 35(8), 569-79.
- Bel’skaya, L.V., Sarf, E.A., Kosenok, V.K. (2018) Correlation interrelations between the composition of saliva and blood plasma in norm. Russian Clinical Laboratory Diagnostics, 63(8), 477-482.
- Fleming, M.V., Klimov, V.V., Cherdyntseva, N.V. (2005) On the interaction of allergic reactions and malignant processes. Siberian Oncology Journal, 13(1), 96-101.
- Keskinege, A., Elgun, S., Yitmaz, E. (2001) Possible implications of arginase and diamine oxidase in prostatic carcinoma. Cancer Detect. Prev, 25 (1), 76-9.
- Manina, I.V., Peretolchina, N.M., Saprykina, N.S., Kozlov, A.M., Mikhailova, I.N., Zhordania, K.I., Barishnikov, A.Y. (2010) Prospects for the use of an H2-histamine receptor antagonist (cimetidine) as an adjuvant of melanoma biotherapy. Immunopathology, allergology, infectology, 4, 42-51.
- Faverio, F., Guzzetti, A., Mereghetti, A., Jemoli, R. (1982) Hiperhistaminemia nelle neoplasie della mammilla. Chirurgia Italiana, 34(5), 727-34.
- Bel’skaya, L.V., Kosenok, V.K. (2018) The level of sialic acids and imidazole compounds in the saliva of patients with lung cancer of different histological types. Siberian journal of oncology, 17(6), 84-91. DOI
- Schuurbiers, O., Meijer, T., Kaanders, J., Looijen-Salamon, M.G., de Geus-Oei, L.F., van der Drift, M.A., van der Heijden, E.H.F.M., Oyen, W.J., Visser, E.P., Span, P.N., Bussink, J. (2014) Glucose Metabolism in NSCLC Is Histology-Specific and Diverges the Prognostic Potential of 18FDG-PET for Adenocarcinoma and Squamous Cell Carcinoma. J Thorac Oncol., 9, 1485–93. DOI
- Swinson, D.E., Jones, J.L., Cox, G., Richardson, D., Harris, A.L., O’Byrne, K.J. (2004) Hypoxia-inducible factor-1 alpha in non-small cell lung cancer: relation to growth factor, protease and apoptosis pathways. Int J Cancer., 111, 43–50. DOI
- Stotz, M., Szkandera, J., Seidel, J., Stojakovic, T., Samonigg, H., Reitz, D., Gary, T., Kornprat, P., Schaberl-Moser, R., Hoefler, G., Gerger, A., Pichler, M. (2014) Evaluation of uric acid as a prognostic blood-based marker in a large cohort of pancreatic cancer patients. PLoS One, 9(8), e104730. DOI
- Chen, Y.F., Li, Q., Chen, D.T., Pan, J.H., Chen, Y.H., Wen, Z.S., Zeng, W.A. (2016) Prognostic value of pre-operative serum uric acid levels in esophageal squamous cell carcinoma patients who undergo R0 esophagectomy. Cancer Biomark, 17(1), 89–96. DOI
- Galunska, B., Paskalev, D., Yankova, T., Chankova, P. (2004) Two-faced Janus biochemistry: uric acid - an oxidant or an antioxidant? Nefrologiya, 4(8), 25–31.
- Christen, S., Bifrare, Y., Siegenthaler, C., Leib, S.L., Tauber, M.G. (2001) Marked elevation in cortical urate and xanthine oxidoreductase activity in experimental bacterial meningitis. Brain Res., 900, 244–51.
- Kopprash, S., Richter, K., Leonardt, W. (2000) Urate attenuates oxidation of native low-density lipoprotein by hydrochlorite and the subsequent lipoprotein-induced respiratory burst activities of polymorphonuclear leukocytes. Molec Cell Biochem, 206, 51–6.
- Malathi, M., Shrinivas, B.R. (2001) Relevance of serum alkaline phosphatase as a diagnostic aid in lung pathology. Indian J Physiol Pharmacol., 45(1), 119–21.
- Dokic-Lisanin, M., Pantovic, V., Jovanovic, Z., Samardzic, G., Jurisic, V. (2013) Values of alkaline phosphatase and their isoenzyme profiles in patients with cancer in respect to bone and liver metastasis. Arch. Oncol., 21(1), 14–6. DOI
- Bel’skaya, L.V., Kosenok, V.K., Massard, G. (2018) Activity of metabolic enzymes of saliva with neuroendocrine tumors of the lung of various degrees of malignancy. Russian Clinical Laboratory Diagnostics, 63(11), 677–82.
- Hussain, S.P., Trivers, G.E., Hofseth, L.J., He, P., Shaikh, I., Mechanic, L.E., Doja, S., Jiang, W., Subleski, J., Shorts, L., Haines, D., Laubach, V.E., Wiltrout, R.H., Djurickovic, D., Harris, C.C. (2004) Nitric oxide, a mediator of inflammation, suppresses tumorigenesis. Cancer Res, 64(19), 6849–53. DOI
- Cheng, H., Wang, L., Mollica, M., Re, A.T., Wu, S., Zuo, L. (2014) Nitric oxide in cancer metastasis. Cancer Letters, 353, 1–7. DOI
- Chanvorachote, P., Pongrakhananon, V., Chaotham, C. (2016) Roles of nitric oxide on cancer stemness and metastasis in lung cancer cells. Asian journal of pharmaceutical sciences, 11, 24–5. DOI
- Thomas, D.D., Heinecke, J.L., Ridnour, L.A., Cheng, R.Y., Kesarwala, A.H., Switzer, C.H., McVicar, D.W., Roberts, D.D., Glynn, S., Fukuto, J.M., Wink, D.A., Miranda, K.M. (2015) Signaling and stress: the redox landscape in NOS2 biology. Free Radic Biol Med, 87, 204–25. DOI
- Heinecke, J.L., Ridnour, L.A., Cheng, R.Y., Switzer, C.H., Lizardo, M.M., Khanna, C., Glynn, S.A., Hussain, S.P., Young, H.A., Ambs, S., Wink, D.A. (2014) Tumor microenvironment-based feed-forward regulation of NOS2 in breast cancer progression. Proc Natl Acad Sci USA, 111(17), 6323–8. DOI
- Cardnell, R.J., Mikkelsen, R.B. (2011) Nitric oxide synthase inhibition enhances the antitumor effect of radiation in the treatment of squamous carcinoma xenografts. PloS One, 6(5), e20147. DOI